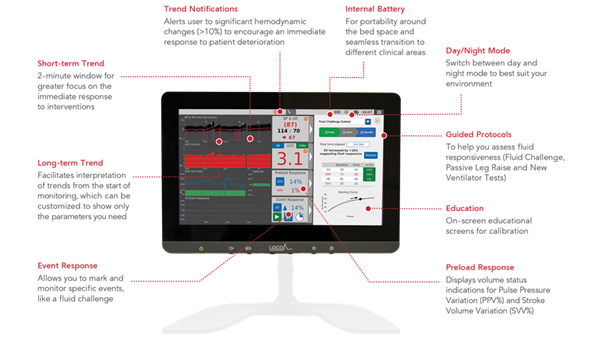
In high-acuity care settings like the operating room, the LiDCO Hemodynamic Monitoring System offers beat-to-beat sophisticated hemodynamic monitoring to enable informed decision-making.
- Monitors hemodynamic parameters using an already-present arterial line and blood pressure transducer.
- The PulseCOTM algorithm scales each patient’s age, height, and weight to transform beat-to-beat blood pressure into its component parts, flow, and resistance.
- Reliable in patients taking vasoactive medications
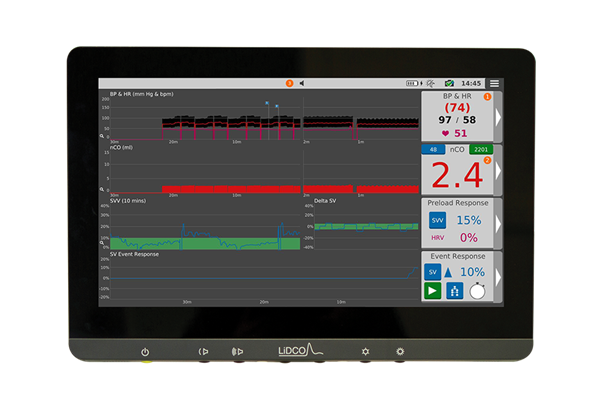
Reductions in Postoperative Complications and Costs
- Hemodynamic optimisation with LiDCO resulted in a 20% decrease in postoperative complications in a randomised controlled trial involving 743 patients having major abdominal surgery. As a result, patients monitored with LiDCO had an average treatment cost of $530 less than control patients who were not monitored.2
Reductions in 30-Day and 180-Day Mortality
- In a study comparing the outcomes of 600 emergency laparotomy patients, researchers discovered that there was a significant drop in mortality at 30 days (from 21.8 to 15.5%) and 180 days (from 29.5 to 22.2%) after the adoption of a programme utilising LiDCO technology.3
The beat–to–beat parameters displayed by the LiDCO monitor provide immediate feedback on a patient’s fluid and hemodynamic status.
The LiDCO monitor provides the following parameters:
- Stroke Volume (SV):The amount of blood pumped by the left ventricle of the heart in one contraction
- Cardiac Output (CO):The amount of blood the heart pumps through the circulatory system in a minute, calculated by multiplying the stroke volume by the patient’s heart rate
- Systemic Vascular Resistance (SVR):Reflects the resistance to flow and is calculated as the quotient of pressure and cardiac output
- Oxygen Delivery (DO2):The amount of oxygen delivered to the tissues, calculated as the product of cardiac output and oxygen concentration
- Stroke Volume Variation (SVV):A dynamic variable that can predict fluid responsiveness in mechanically ventilated patients, SVV is the variation in stroke volume across at least one respiratory cycle
- Pulse Pressure Variation (PPV):Another dynamic variable that can predict fluid responsiveness in mechanically ventilated patients, PPV is the variation in arterial pulse pressure across at least one respiratory cycle